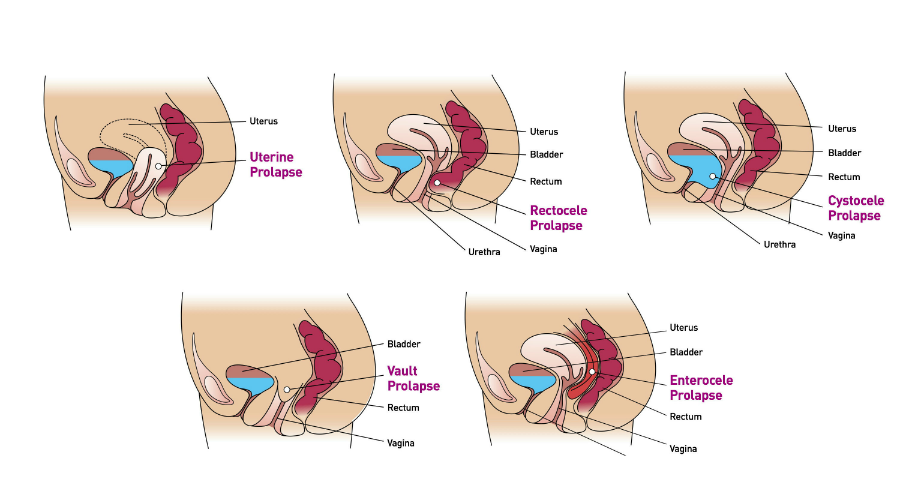
Most women after a vaginal delivery experience some trauma and damage to the supportive structure of their vagina. These supportive structures are scaffolding that maintains the position and the proper functioning of the organs surrounding the vagina, such as bladder, uterus, and the rectum.
Significant damage to the musculature and connective tissues supporting the vaginal organs causes disruption in urination and bowel movement control. Women with urinary incontinence issues report urinary urgency and frequency, loss of urine on the way to the bathroom, difficulty emptying the bladder, urine loss with exercise or any type of straining, multiple trips for urination to the bathroom, constipation, and difficulty emptying the bowel or difficulty controlling gas or stool.
RELATED: Urinary Incontinence Treatment in Los Angeles
Damage to the supportive structures creates bulging of the bladder, uterus, and the rectum into the vagina and sometimes beyond the opening of the vagina. This bulging is mostly palpable when standing or straining. It is reduced when lying down. Sometimes women complain of lower back pain. In severe cases, women find that they have to manually push the prolapsed organ back inside the vagina in order to start or complete the evacuation.
The most common complaint besides the loss of control of urine (urinary incontinence) or stool is palpation of the bulge and the associated discomfort. Most patients restrict their activities in order to avoid leakage and odor and wetness associated with it. Also, some avoid intercourse due to the pain and discomfort as well as reduced sexual confidence due to the vaginal prolapse.
Atrophy of the vaginal tissue after menopause when ovaries no longer produce estrogen also causes further weakness. Dryness associated with lack of hormones and weakness in the supportive connective tissue contributes to further vaginal prolapse and irritability of the bladder and the vagina.
RELATED: Prolapse Treatment in Los Angeles
Dr. Tahery has been involved in many of the clinical studies instrumental in designing new and minimally invasive treatments for urinary incontinence and vaginal prolapse. The majority of the current procedures aims at restoring the vaginal structure and return function using the woman’s own tissues. In most cases, no visible incision is created and all the surgery is performed through the vaginal opening. If needed laparoscopic procedures can be performed to help those that are not good candidates for vaginal surgery. These procedures in most cases are outpatient with little downtime.