Stress Urinary Incontinence (SUI) as defined as involuntary leakage of urine on exertion (ie. sneezing or coughing). It affects approximately 23% to 38% of the female population in the united states over the age of 20. It is estimated 7% to 10% are severe with frequent leakage. Yearly only 10% of women diagnosed with incontinence undergo surgical correction. The incidence of urinary incontinence increases with age and has become more common with increasing age of the US population.
Vaginal birth is a major cause of stress urinary incontinence (SUI) in women. 33% of women at postpartum complain of SUI and a significant number continue to suffer at five years were found to be dealing with SUI.
During vaginal delivery, the head of the infant enters the vaginal canal, stretching and tearing the hammock like supporting structures that make up the urinary continence mechanism. A vaginal delivery also decreases pelvic floor muscle strength and causes significant muscle damage. Pelvic nerve injury is also common in incontinent women after vaginal delivery. Weakness because of partial nerve damage of the pelvic floor sphincter muscle and the pudendal nerve is a common finding in women after childbirth. Also, damage to the supportive structures and loss of the ability to perform pelvic floor muscle contraction has been shown in postpartum women with SUI.
Vaginal delivery doubles chances of urinary incontinence, and with increasing parity, the prevalence of urinary incontinence also increases. Antepartum urinary incontinence is a predictor of postpartum incontinence and routine episiotomy has not found to be protective. The role of other obstetric factors such as prolonged pushing, increased head circumference, high birth weight, epidural anesthesia, and oxytocin use is still being looked at as a cause of SUI.
Besides obstetric injury, any other chronic pressure can lead to stress incontinence. Obesity, chronic cough, lung disease, chronic constipation, and high-impact exercise can all cause stress incontinence. Radiation can cause stress incontinence by damaging and scarring the bladder and its support. Also, certain people may be more likely to develop stress incontinence due to their genetic makeup.
The main goals in evaluating stress incontinence are to eliminate other bladder conditions and confirming the loss of urine with stress. A detailed history and examination are essential to the correct diagnosis. Also testing in the office including cystoscopy, urodynamic testing, and other modalities are used to help guide our treatment options.
Non-surgical treatment options are used whenever possible to treat or improve the results of surgical repair. Biofeedback is used to teach correct contractions of the pelvic floor muscles, and electrical stimulation is used to exercise muscles that are damaged and beyond the patient’s ability to contract. Biofeedback is effective in treatment for urinary incontinence. Treatment sessions usually are weekly for 6-8 weeks and last about a ½ hour.
Transurethral injections, sling operations, Burch procedure, are outpatient procedures available for surgical treatment of SUI. In patients diagnosed with SUI, surgical success can be as high as 85%. In general, the recovery and downtime from these operations are short and postoperative pain minimal.
As a urogynecologist, Dr. Tahery is an expert in diagnosing and treating urinary incontinence and related conditions.
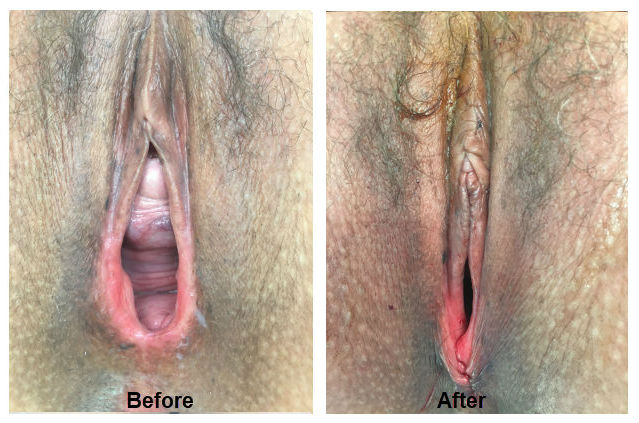
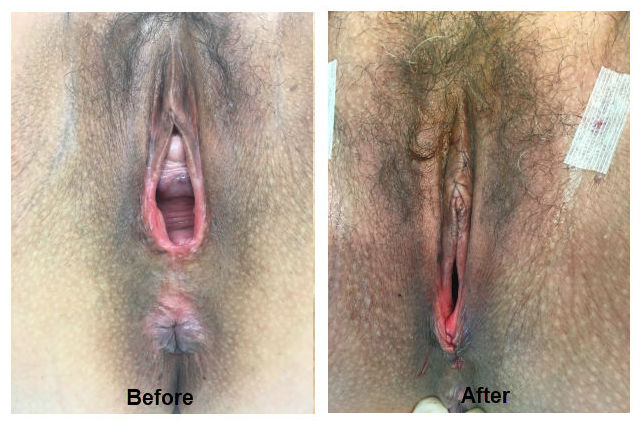
Case Study
This patient is a 36 year old female with two uncomplicated vaginal deliveries, complained of stress urinary incontinence, pressure with exercise, and lack of sensation during intercourse. The before pictures show a gaping opening of the vagina, reflecting damage to the internal and external supportive structures, poor tone in the muscles and connective tissue supporting the bladder and the rectum. This patient underwent a sling operation, and a total reconstruction of the vaginal support tissue, as well as cosmetic repair of the vaginal opening. This patient was discharged home the same day of the operation and was back to work in one week.